
 乳腺癌易感基因的多基因检测已经广泛开展于欧美,但是亚洲相对较少。
乳腺癌易感基因的多基因检测已经广泛开展于欧美,但是亚洲相对较少。
2018年5月12日,国际抗癌联盟《国际癌症杂志》在线发表中国19家机构研究报告,对中国26个中心937例高遗传风险乳腺癌患者包括BRCA1和BRCA2在内的40个乳腺癌易感基因种系突变情况进行了大数据分析。
作者单位
陆军军医大学第一附属医院(第三军医大学西南医院)
安诺优达基因科技(北京)有限公司
福建省肿瘤医院
新疆医科大学附属肿瘤医院
山西省肿瘤医院
海军军医大学第一附属医院(第二军医大学长海医院)
辽宁省肿瘤医院
吉林省肿瘤医院
首都医科大学附属北京朝阳医院
西安交通大学第一附属医院
广东省人民医院(广东省医学科学院)
解放军第二〇二医院
重庆医科大学附属第二医院
空军军医大学第一附属医院(第四军医大学西京医院)
陆军军医大学第三附属医院(第三军医大学大坪医院)
哈尔滨医科大学附属第二医院
湖南省肿瘤医院(中南大学湘雅医学院附属肿瘤医院)
四川省人民医院
河南省肿瘤医院
该研究于2015~2016年从中国26个中心连续入组高遗传风险乳腺癌患者937例,收集临床信息,并对参与者血液标本进行高通量二代测序以确定种系(多细胞动物繁殖后代的细胞总称,包括单倍体配子以及最终能分化成配子的原始生殖细胞)基因突变。该研究由中国健康促进基金会提供资助。
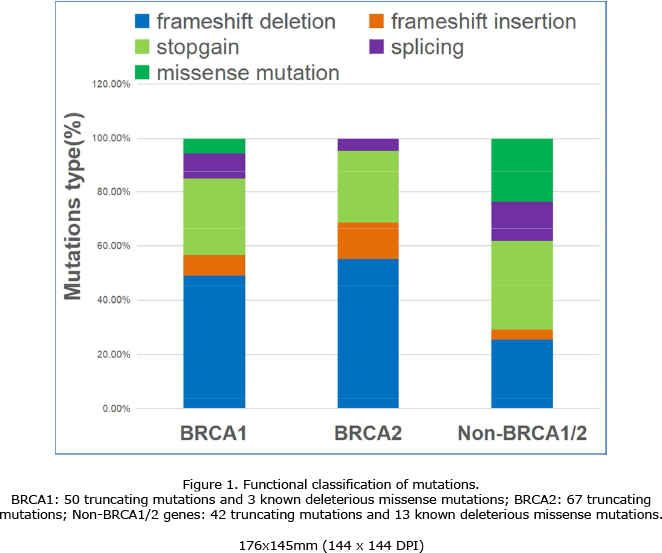
结果发现种系基因突变223例:
BRCA1/2基因突变159例
15个其他乳腺癌易感基因突变61例
BRCA1/2和非BRCA1/2基因突变3例
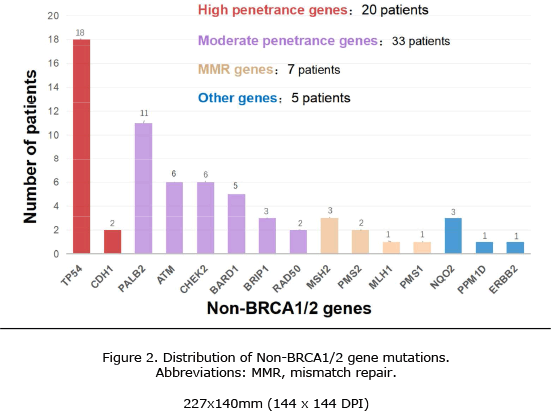
主要的非BRCA1/2基因突变:
TP53基因突变18例
PALB2基因突变11例
CHEK2基因突变6例
ATM基因突变6例
BARD1基因突变5例
整体而言,并未发现非BRCA1/2基因病理突变的预测因素,除了:
HER2阳性乳腺癌患者TP53突变率较高
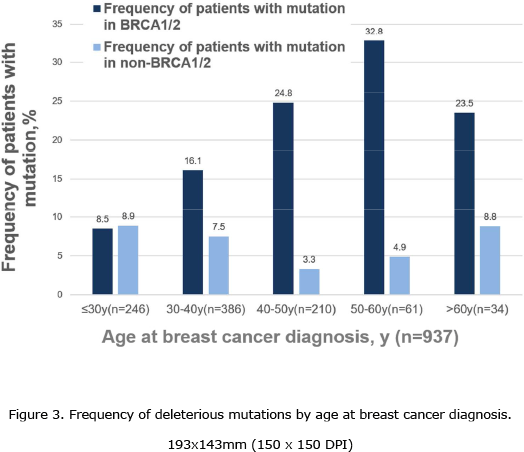
诊断时年龄较轻患者TP53突变率较高
管腔型乳腺癌患者CHEK2和PALB2突变率较高
对于中国高遗传风险乳腺癌患者,种系突变占23.8%,其中非BRCA1/2基因突变占6.8%,TP53和PALB2的突变率较高(1.9%和1.2%)。
因此,该研究虽然并未发现非BRCA1/2基因有害突变的预测因素,但是具有某些临床特征患者的若干特定基因突变率较高。
Int J Cancer. 2018 May 12. [Epub ahead of print]
Germline mutations in 40 cancer susceptibility genes among Chinese patients with high hereditary risk breast cancer.
Li J, Jing R, Wei H, Wang M, Qi X, Liu H, Liu J, Ou J, Jiang W, Tian F, Sheng Y, Li H, Xu H, Zhang R, Guan A, Liu K, Jiang H, Ren Y, He J, Huang W, Liao N, Cai X, Ming J, Ling R, Xu Y, Hu C, Zhang J, Guo B, Ouyang L, Shuai P, Liu Z, Zhong L, Zeng Z, Zhang T, Xuan Z, Tan X, Liang J, Pan Q, Chen L, Zhang F, Fan L, Zhang Y, Yang X, Li J, Chen C, Jiang J.
Southwest Hospital, Third Military Medical University, Chongqing, China; Annoroad Gene Technology (Beijing) Co. Ltd, Beijing, China; Fujian Provincial Cancer Hospital, Fuzhou, Fujian, China; Affiliated Tumor Hospital of Xinjiang Medical University, Urumqi, Xinjiang, China; Shanxi Cancer Hospital, Taiyuan, Shanxi, China; Changhai Hospital, Second Military Medical University, Shanghai, China; Liaoning Cancer Hospital and Institute, Shenyang, Liaoning, China; Jilin Cancer Hospital & Institute, Changchun, Jilin, China; Beijing Chaoyang Hospital Affiliated to Capital Medical University, Beijing, China; First Affiliated Hospital of Xi'an Jiaotong University, Xi'an, Shaanxi, China; Cancer Center, Guangdong General Hospital, Guangdong Academy of Medical Sciences, Guangzhou, Guangdong, China; PLA No.202 Hospital, Shenyang, Liaoning, China; Second Affiliated Hospital of Chongqing Medical University, Chongqing, China; Xijing hospital, Forth Military University, Xi'an, Shaanxi, China; Research Institute of Surgery, Third Military Medical University, Chongqing, China; Second Affiliated Hospital of Harbin Medical College, Harbin, Heilongjiang, China; Hunan Cancer Hospital, Affiliated Cancer Hospital of Xiangya School of Medicine, Central South University, Changsha, Hunan, China; Sichuan Provincial People's Hospital, Chengdu, Sichuan, China; Henan Cancer Hospital, Zhengzhou, Henan, China.
Multigene panel testing of breast cancer predisposition genes have been extensively conducted in Europe and America, which is relatively rare in Asia however. In this study, we assessed the frequency of germline mutations in 40 cancer predisposition genes, including BRCA1 and BRCA2, among a large cohort of Chinese patients with high hereditary risk of BC. From 2015 to 2016, consecutive BC patients from 26 centers of China with high hereditary risk were recruited (n=937). Clinical information was collected and next-generation sequencing (NGS) was performed using blood samples of participants to identify germline mutations. In total, we acquired 223 patients with putative germline mutations, including 159 in BRCA1/2, 61 in 15 other BC susceptibility genes and 3 in both BRCA1/2 and non-BRCA1/2 gene. Major mutant non-BRCA1/2 genes were TP53 (n=18), PALB2 (n=11), CHEK2 (n=6), ATM (n=6), and BARD1 (n=5). No factors predicted pathologic mutations in non-BRCA1/2 genes when treated as a whole. TP53 mutations were associated with HER-2 positive BC and younger age at diagnosis; and CHEK2 and PALB2 mutations were enriched in patients with luminal BC. Among high hereditary risk Chinese BC patients, 23.8% contained germline mutations, including 6.8% in non-BRCA1/2 genes. TP53 and PALB2 had a relatively high mutation rates (1.9% and 1.2%). Although no factors predicted for detrimental mutations in non-BRCA1/2 genes, some clinical features were associated with mutations of several particular genes.
KEYWORDS: Breast Cancer; Cancer Susceptibility Genes; Chinese Population; Germline Mutations; Multiple-gene sequencing
PMID: 29752822
DOI: 10.1002/ijc.31601











 苏公网安备32059002004080号
苏公网安备32059002004080号


